Intraocular Lenses
An intraocular lens, commonly called an IOL, is a tiny artificial lens for the eye
An IOL permanently replaces the eye’s natural lens when it is removed during cataract surgery.
Why is the eye’s natural lens removed during cataract surgery?

Intraocular lens implant replaces your natural lens.
Normally, the eye’s natural lens is clear, allowing light to pass through and focus on the retina. When a cataract forms, the lens becomes cloudy, and light can no longer remain sharply focused when it passes through the lens to the retina. As a result, vision becomes blurred. The only way to treat a cataract is by removing the clouded lens itself.
Can I see clearly without a lens?
No, the eye cannot focus properly without a lens. Thick eyeglasses, a contact lens or an intraocular lens must be substituted to restore the eye’s focusing power. Because an IOL is a permanent replacement for the natural lens, it is used in the majority of all cataract surgery patients. The IOL provides better vision than thick eyeglasses do, and it is much more convenient than a contact lens because it doesn’t have to be taken on and off the eye.
How will an IOL affect my vision?
IOLs come in different focusing powers, just as contact lenses or prescription eyeglasses do. Your ophthalmologist (Eye M.D.) will perform a special preoperative evaluation of your eye to determine the proper power of the lens implant. The length of your eye and the curvature of your cornea are measured with special instruments. Your ophthalmologist then uses these measurements to calculate the correct focusing power of the IOL.
The natural lens of your eye has the ability to change shape in order to focus at varying distances. The IOL, which cannot change shape, can be calculated to see clearly up close, at mid-range, or at long range. In most cases, you will wear thin glasses to allow you to see all distances in focus. There are newer IOLs, which allow for different focusing powers within the same lens. With these multifocal or accommodative IOLs, it is possible to see more clearly at various distances than monofocal or fixed-focus lenses. You should discuss these possibilities with your eye surgeon, and together, you will decide which lens is right for you.
In most cases you should notice significant improvement in vision after cataract surgery.
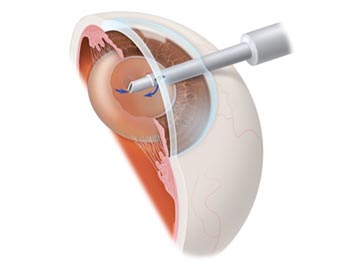
Small instruments gently remove the yellowed natural lens (cataract).
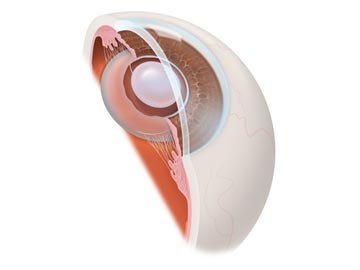
The implanted IOL is seen centered and behind the iris, taking the place of the natural lens.
Where will the IOL be placed?
An IOL is placed in the center of the pupil, either in front of or behind the iris (the colored part of your eye). It is most commonly placed behind the iris where the natural lens was located.
What is the IOL made of?
Most of the IOLs implanted today are made of silicone or acrylic materials. These lenses can be folded and inserted through a small (approximately 3 millimeter)incision during cataract surgery. In the past, IOLs have been made of hard plastic, similar to a hard contact lens.
Will the IOL ever need to be replaced?
IOL implants are well tolerated by the eye and are intended to last for a lifetime. Only rarely do the lenses need to be removed and replaced.
What are the risks of IOL implantation?
The success rate of cataract surgery with an IOL implant is excellent, resulting in improved vision in the majority of patients. A small number of patients may have problems, though they may not be caused by the IOL itself. Complications following cataract surgery may include:
- Infection
- Bleeding
- Swelling of the cornea
- Detachment of the retina
- Damage to the iris or pupil
Be sure to discuss potential complications with your ophthalmologist before surgery.
Monofocal Lens
Multifocal Lens
Accomodative Lens
Toric Lens
Multifocal Toric Lens
Accomodative Toric Lens
- Anatomy of the Eye
- Botox
- Cataracts
- Diabetes and the Eye
- Diabetic Retinopathy – What is it and how is it detected?
- Treatment for Diabetic Retinopathy
- Non-Proliferative Diabetic Retinopathy (NPDR) – Video
- Proliferative Diabetic Retinopathy (PDR) – Video
- Cystoid Macular Edema
- Vitreous Hemorrhage – Bleeding from diabetes (Video)
- Vitrectomy Surgery for Vitreous Hemorrhage (Video)
- Macular Edema
- Laser Procedures for Macular Edema (Video)
- Laser for Proliferative Diabetic Retinopathy – PDR (Video)
- How the Eye Sees (Video)
- Dilating Eye Drops
- Dry Eyes and Tearing
- Eye Lid Problems
- A Word About Eyelid Problems
- Bells Palsy
- Blepharitis
- Blepharoptosis – Droopy Eyelids (Video)
- Dermatochalasis – excessive upper eyelid skin (Video)
- Ectropion – Sagging Lower Eyelids (Video)
- Entropion – Inward Turning Eyelids (Video)
- How to Apply Warm Compresses
- Ocular Rosacea
- Removing Eyelid Lesions
- Styes and Chalazion
- Twitches or Spasms
- Floaters and Flashes
- Glaucoma
- Selective Laser Trabeculoplasty (SLT) for Glaucoma
- Glaucoma: What is it and how is it detected?
- Optical Coherence Tomography OCT – Retina & Optic Nerve Scan
- Treatment for Glaucoma
- Retinal Nerve Fibers and Glaucoma (Video)
- Open Angle Glaucoma (Video)
- Closed Angle Glaucoma (Video)
- Visual Field Test for Glaucoma
- Glaucoma and Blind Spots (Video)
- Treatment for Glaucoma with Laser Iridotomy (Video)
- Laser Treatment for Glaucoma with ALT and SLT (Video)
- Surgical Treatment for Glaucoma with Trabeculectomy (Video)
- Surgical Treatment of Glaucoma with Seton (Video)
- Keeping Eyes Healthy
- Laser Vision Correction
- Latisse for Eyelashes
- Macular Degeneration
- Macular Degeneration – What is it and how is it detected?
- Treatment for Macular Degeneration
- Dry Macular Degeneration (Video)
- Wet Macular Degeneration (Video)
- Treatment of Macular Degeneration with Supplements
- Treatment of Wet Macular Degeneration with Anti-VEGF Injections
- Amsler Grid – A home test for Macular Degeneration (Video)
- Living with Vision Loss
- How the Eye Works – The Macula (Video)
- Other Eye Conditions
- Central Serous Retinopathy
- Lattice Degeneration of the Retina
- A Word About Other Eye Conditions
- Amblyopia
- Carotid Artery Disease and the Eye
- Fuch’s Corneal Dystrophy
- Herpes Simplex and the Eye
- Herpes Zoster (Shingles) and the Eye
- Ischemic Optic Neuropathy
- Keratoconus
- Macular Hole
- Macular Pucker
- Microvascular Cranial Nerve Palsy
- Migraine and the Eye
- Optic Neuritis
- Pseudotumor Cerebri
- Retinal Vein Occlusion
- Retinitis Pigmentosa
- Retinopathy of Prematurity
- Strabismus
- Thyroid Disorders and the Eye
- Uveitis
- Vitreomacular Adhesions / Vitreomacular Traction Syndrome
- Red Eye
- Refractive Errors
- Retinal Tears and Detachments
Disclaimer
This Patient Education Center is provided for informational and educational purposes only. It is NOT intended to provide, nor should you use it for, instruction on medical diagnosis or treatment, and it does not provide medical advice. The information contained in the Patient Education Center is compiled from a variety of sources. It does NOT cover all medical problems, eye diseases, eye conditions, ailments or treatments.
You should NOT rely on this information to determine a diagnosis or course of treatment. The information should NOT be used in place of an individual consultation, examination, visit or call with your physician or other qualified health care provider. You should never disregard the advice of your physician or other qualified health care provider because of any information you read on this site or any web sites you visit as a result of this site.
Promptly consult your physician or other qualified health provider if you have any health care questions or concerns and before you begin or alter any treatment plan. No doctor-patient relationship is established by your use of this site.

